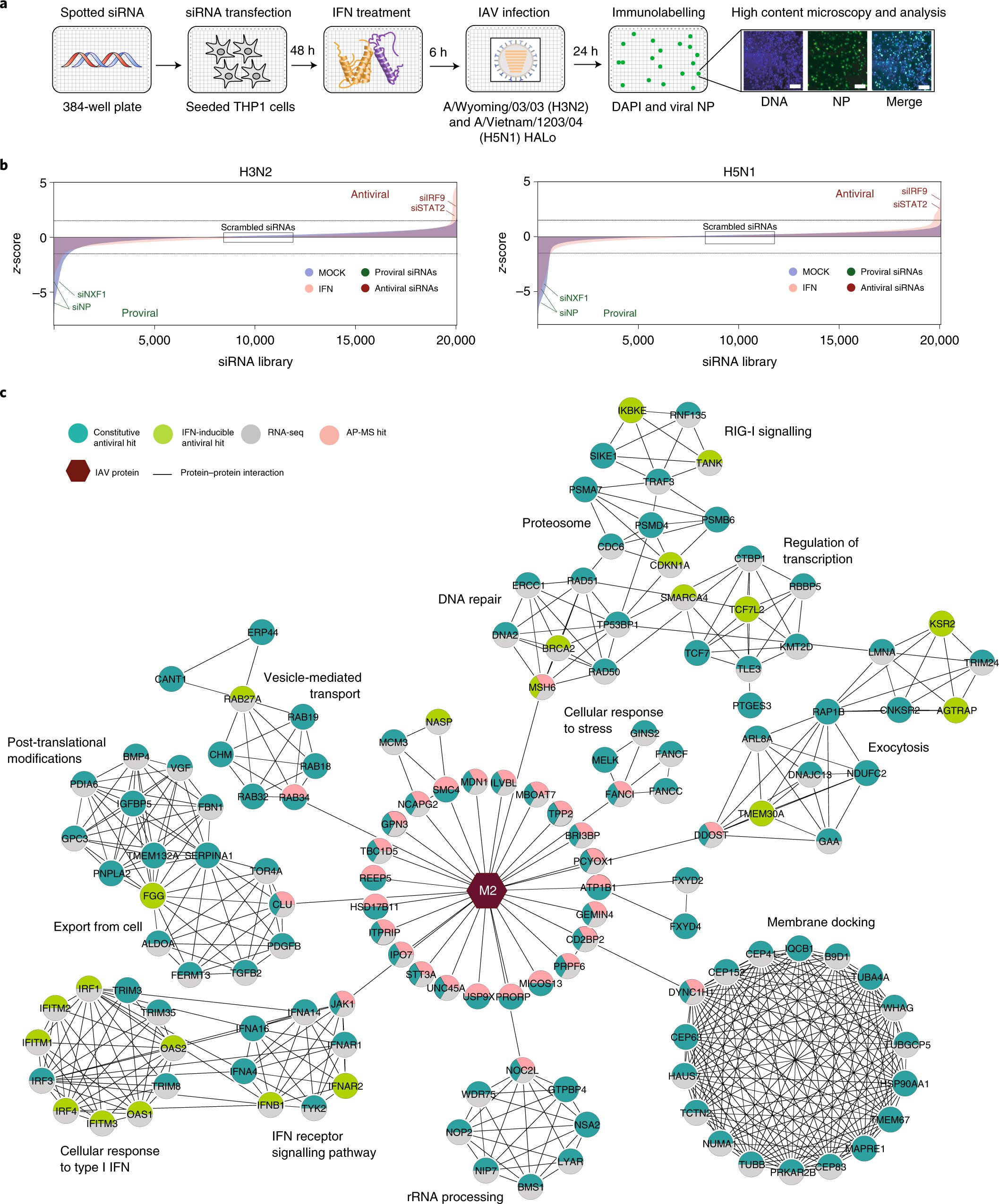
Fig. 1: Multi-omics analysis IAV cellular restraint. Schematic representation of the genome wide siRNA screen to identify cell factors that affect IAV replication. b, The genome-wide siRNA screen ranked the z-scores (blue, mock-treated cell; pink, IFN treated cells). Dashed lines show the z score cut-off. zcore >1.5 means that there are antiviral factors. zcore
According to Nature Microbiology, human cells use TBC1D5 protein to route influenza A viruses into host cells. This prevents the virus from spreading to other cells.
Although influenza viruses have their own ways of defeating host defenses, pharmacological strategies to increase host defenses could be one way of developing new anti-viral treatments, says Judd Hultquist (Ph.D.), assistant professor of Medicine in Division of Infectious Diseases, and co-author of this study.
Hultquist stated that "this is one of the great dreams in virology to identify host-targeted therapeutic approaches that limit the risk for antiviral resistance but have pan-viral potential."
The influenza A virus is a very successful virus. The virus infects more than 20,000,000 people annually in the United States. It has developed sophisticated methods to infect human cells and turn them into virus-producing factories. Although viruses can also be prevented by cells, they evolve and adapt faster than human cells.
Hultquist stated that they were interested in the arms race between host and virus.
Hultquist and his collaborators from the Sanford Burnham Prebys Medical Discovery Institute used an automated screening platform to knock down almost every gene in the human genome. They also measured the impact of viral infection on the screen. Hultquist explained that when antiviral proteins get knocked down, it causes an increase in infection.
Researchers identified many genes that inhibit viral replication. However, TBC1D5 was the most important because of its role in autophagy (a process where host cells recycle their protein). TBC1D5 can disrupt the process of transporting new viruses from the inside to the outside cells. It flags the viruses as trash and orders them to be destroyed if it is overexpressed. This mechanism fails in most cases, even when TBC1D5 is not overexpressed in normal people.
The virus has a counterattack. A protein that binds with the TBC1D5 flag and nullifies the host defense is what this does.
Hultquist stated that the virus had created an off switch to facilitate this recycling mechanism. "Our cells are equipped with all the smart defenses we need, but viruses that have been successful have found a way to outwit us and overcome these obstacles."
These critical interactions between host, pathogen and immune system are crucial to developing antiviral therapies that help people fight infections. For example, a small-molecule inhibitor that negates the viral counterattack and increases the effectiveness of the TBC1D5 defense is one way.
It is possible that similar viruses may use the same defense strategies. Many respiratory viruses like influenza viruses, SARS CoV-2, and respiratory syncytial viruses (RSV), rely on unique architectures of respiratory cells to reproduce. Hultquist suggested that it is possible that each of them has found unique ways to break through this replication block.
Hultquist stated that if we can find these common elements, we can start developing pan-viral therapies.
Learn more about the Ebola-fighting protein found in human cells
Additional information: Laura Martin Sancho et., Restriction Factor Compendium for Influenza A Virus reveals a mechanism to evade autophagy Nature Microbiology (2021). Information from Nature Microbiology Laura Martin Sancho et. al., Restriction Factor Compendium for Influenza A virus reveals a mechanism to evade autophagy. (2021). DOI: 10.1038/s41564-021-00964-2
